You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Consistent results in many high-quality clinical trials and clearance by the US Food and Drug Administration have driven a reemergence of interest in 38% silver diamine fluoride (SDF) for managing dental caries. Ease of use and low material cost create the opportunity for fundamental change in first-line management of caries. The implications of non-invasive treatment for the individual practice and improvement of worldwide public health have kept the discussion of SDF on the arrest of active lesions. Indeed, a recent meta-analysis concluded arrest of caries by SDF is supported by high levels of evidence.1 However, SDF also appears to be the most cost-effective approach for preventing caries lesions beyond water fluoridation, surpassing all other fluorides. This article reviews the history of use of SDF, clinical studies, and the material's cost-effectiveness, safety, and esthetics, in development of best practice recommendations.
History
The use of SDF for managing dental caries was pioneered by Nishino, Yamaga, and others in Japan in the 1960s. Their original intent was for prevention: "both [silver and fluoride] ions increase the resistance of enamel to dental caries."2 Indeed, the first experiments using SDF were studies in a rat caries model where the investigators evaluated the incidence of new lesions after preventive application. In the very first study, SDF prevented 62% of caries lesions in the molars of treated rats compared to littermate controls. SDF decreased the severity of lesions as well: 30% of teeth in the control group developed deep lesions (rat caries index 2 and 3), while none of the teeth in the SDF group had any.3 The second rat model caries study elucidated (to some extent) the benefit of both silver and fluoride ions in the preventive effect: SDF treatment resulted in 65% less new lesions than no treatment control, while 10% stannous fluoride (SnF2) prevented only 51%, and 25% silver nitrate had no effect.4
The one early human clinical trial documenting the powerful preventive effect on caries lesions was a split-mouth study in the permanent lower first molars of 25 children ages 6 to 8. Nine months after three SDF treatments within 1 week, 24% of treatment side molars had developed new lesions while 88% did on the untreated side, a 73% reduction.5
After three decades of infrequent studies, contemporary clinical trials with more rigorous experimental designs evaluated the effectiveness of SDF in the management of dental caries. The first two such trials focused on caries arrest in young children but also evaluated the incidence of new lesions as a secondary outcome. In one study, patients treated with SDF had 0.37 new carious surfaces (decayed/missing/filled surfaces [DMFS]), while patients in the control group had 1.58.6 In the other study, these numbers were 0.67 (DMFS) and 2.46.7 The prevented fractions (percent less new lesions) were 77% and 73% after 2.5 years. These impressive results fueled five more trials since, reviewed in the text below.
Open issues that motivate this review include: whether the preventive effect is consistent across clinical trials, whether silver contributes to prevention beyond fluoride, how the effectiveness and cost-effectiveness of SDF compares to other methods and materials, the safety and side effects of SDF, and what the optimal application protocol and frequency should be.
Systematic Literature Review
A literature review was designed to search NIH NCBI PubMed with the following search terms: ("33040-28-7" OR "1Z00ZK3E66" OR "silver diamine fluoride" OR "silver fluoride" OR "diammine silver fluoride" OR "ammonical silver fluoride" OR "ammoniacal silver fluoride" OR ["silver" AND "fluoride"]) AND ("prevention" OR "incidence" OR "prevent") AND (["caries" OR "clinical" OR "trial" OR "in vivo"] OR ["enamel" OR "incipient" OR "white spot" OR "pit" OR "fissure"]). Meta-analyses and other systematic reviews identified by the search were scoured for any missed primary articles.2,8,9 Papers not published in English were translated as necessary.
A total of 114 papers were retrieved. Titles and abstracts were evaluated by the first author (JAH) for: (A) human clinical studies with incidence of new caries lesions as an outcome, and (B) clinical studies on the progression of enamel lesions into dentin. All other papers were considered based on clinical relevance, which identified two papers on cost-effectiveness and two on patient preference. Most papers were reviews or other opinion pieces without primary data. No meta-analysis was found that summarized the preventive effects of SDF.
Prevention
Seventeen papers described human clinical studies with prevented caries lesions as an outcome. The study design and reporting of these studies vary considerably in their risk of biases. The clinical caries studies (n = 15) focused on the use of SDF in children 1 to 12 years old (yo) or adults 60 yo and older (n = 3). Of these, one case series of 12% SDF on newly erupted molars in 120 children 5.5 to 6 yo found no new lesions after 1 year but included no control group.10 One paper describing 83% caries arrest in children 0 to 2 yo a year after treatment with 30% SDF noted in the discussion a strong inverse correlation between the arrest of caries and the incidence of new lesions in each patient, but did not publish the actual data.11 The titles of three other papers suggest that they may be relevant, but were not accessible to the present authors.12-14 Three high-quality trials have been performed in elders and will be discussed elsewhere.15,16 The remaining nine papers described comparative studies on the incidence of new caries lesions after the use of 38% SDF or 40% silver fluoride (AgF) versus no treatment or placebo control groups in children. These papers are summarized below.
Children
Nine studies evaluated prevention of new lesions in children. The outcomes and design of these studies are summarized in Figure 1.5-7,12-17 The Japanese nonrandomized split-mouth study in 25 children 6 to 8 yo described above showed 73% less new lesions compared to 0.88 mean new lesions in the control group.5 A similar split-mouth study in 26 toddlers 1 to 2 yo randomized quadrants to SDF versus control separately by upper and lower arch. While caries arrest was observed for existing lesions in the SDF group, no prevention with respect to the untreated side (2.2 new lesions) was observed at any timepoint from 3 to 12 months. This outcome is an outlier with respect to other studies (Figure 1); it is possible that isolation was not achieved between occluding SDF-treated and control teeth.12
Another randomized split-mouth study examined the effect of SDF on proximal surfaces of primary molars with and without existing enamel lesions in 58 children 5 to 7 yo. SDF was applied and examined every 3 months clinically and radiographically. After 18 months, 56% less lesions were observed in SDF-treated upper teeth and 71% less in lower teeth, with respect to the contralateral control (the quantity of lesions was not reported).13 A study of 849 children 5 to 8 yo in Australia evaluated the incidence of new lesions in newly erupted first permanent molars after 10% SnF2 only versus placement of 40% AgF followed by 10% SnF2. Each treatment was performed once only, with one treatment modality per each of two nearby clinics that served socioeconomically similar patients. Relative to 11.7 new lesions in the control group, after 18 months patients treated with SDF had 76% less new lesions.14
Four contemporary randomized controlled trials studied prevention by SDF compared to placebo or no treatment controls. In the first, after 2.5 years 77% less new lesions were observed in the anterior teeth of 308 children 3 to 5 yo whose lesions were treated with SDF once per year and 50% in those who were treated topically with 5% sodium fluoride varnish four times per year, with respect to the average of 1.6 new lesions of those who received a water placebo.6 The next study found 73% less new lesions in the primary and permanent molars of 373 children initially 6 yo after 3 years of twice-per-year SDF treatment to lesions only, as compared to 2.5 new lesions in no treatment controls.7 A third study in 708 children 6 to 8 yo found the incidence of new lesions 18 months after a single placement of SDF or a glass-ionomer sealant in permanent first molars to be 23% and 70%, respectively, less than no treatment controls, who had 0.44 new lesions.15 The fourth study evaluated the incidence of new lesions in permanent first molars of 482 children 9.1 yo, 2 years after a single placement of a resin sealant, annual application of SDF, or twice annual fluoride varnish, to be 65%, 52%, and 48%, respectively, less than the 4.6 new surfaces of caries lesions in the placebo control.16
The most recent published clinical study evaluated SDF in 295 children 2 to 3 yo. This study used as its control group children who were part of the overarching prevention program but were not consented for SDF treatment. Examiners were not blinded. Initial lesions in all groups were similar. All three groups received 2% sodium fluoride gel every 6 months. SDF was placed on caries lesions only, either once or twice annually. After a year the SDF treatment groups had 55% and 57% less new lesions on primary tooth surfaces, compared to 9 new lesions in controls.17
Enamel Lesions
Treatment of lesions limited to enamel and not involving the dentin, also known as incipient lesions, demineralization spots, or white-spot lesions, with the goal of stopping progression into dentin, is within the spectrum of prevention. Four studies were found on this topic. In three studies the control group showed no disease progression18; in two, differences were seen in how quickly lesions became arrested, but final outcomes were similar.19,20 The positive outcomes in control groups shows that the overwhelming majority of enamel lesions in patients with access to care will not grow in 2 to 3 years and, therefore, should be not be treated operatively at this stage. One of these clinical trials found that treatment with SDF was more comfortable and quicker than with infiltration resin. SDF treatment was no different in terms of discomfort than flossing instructions.21
Only one study documented the progression of enamel lesions into dentin in control groups. In the randomized split-mouth study of 58 children 5 to 7 yo mentioned earlier, after 18 months 46% less initial lesions in upper primary molars and 59% less initial lesions in lower primary molars progressed into the dentin after application of SDF every 3 months compared to controls.13 Data on the numbers of lesions that grew in the control teeth were not reported, so it is impossible to fully evaluate the magnitude of the clinical effects.
Summary of Clinical Trial Evidence
These clinical studies can be summarized as demonstrating clinically significant prevention of effects of new caries lesions in children in primary and permanent teeth. Moreover, the prevention trials, conducted in varying populations by a range of investigators, showed a strongly consistent prevented fraction of 61% in children (Figure 1). This means a patient treated with SDF will have 61% less new lesions than if he or she had not received SDF.
In Figure 2 the number of children included in the summary analysis (SDF and control groups) is plotted against the prevented fraction observed in each study. This type of plot characterizes the overall trend in clinical outcomes and is expected to appear as an upward-pointing funnel converging on the true clinical effect. The estimate of 61% prevented fraction appears reasonable.
Sufficient data was presented in the papers to perform a "number needed to treat" (NNT) analysis for three studies on prevention of lesions by surface on any tooth.6,7,17 While permanent molars were considered in one of these studies, the majority of teeth treated were deciduous (DMFS). Assuming all relevant teeth were present in all patients, the NNT for these studies is 19.9 surfaces, or 4 teeth. This means that only a single child needs to be treated with SDF to prevent one new lesion in primary teeth. Sufficient data were also available from three studies on the prevention of carious first permanent molars (decayed/missing/filled teeth [DMFT]); the NNT is 12.1 teeth.5,14,16 Therefore, three children need to be treated to prevent one carious permanent first molar.
Unlike the trend the authors have observed in increasing rates of caries arrest over time,22,23 no such pattern is observed with caries prevention (Figure 1). The preventive effect of SDF appears to be immediate and long-lasting.
Comparison to Other Topical Preventive Agents
In direct comparison with four times applications per year of 5% sodium fluoride varnish in young children, once annual application of SDF showed significantly higher prevented fraction.6 This exact result was duplicated in a large study of elders.24 However, another study showed no significant differences between twice annual fluoride varnish and once annual SDF.16 These results suggest that one application of SDF per year is at least as effective as two to four applications of fluoride varnish per year, and may be more so.
Comparison to Sealants
Application of SDF for preventing new lesions on newly erupted permanent first molars has been compared directly to dental sealants. In one study, a non-significant trend was observed for higher prevented fraction compared to controls by resin sealants.16 In another, there was a much greater prevented fraction by glass-ionomer sealants than SDF.15 Functionally, SDF-mediated prevention likely depends on continued application over the years as it does with other fluorides25 and as is the case with SDF-mediated caries arrest.26 Sealants need to be monitored at a similar frequency.27 Maintenance of SDF treatments and sealant monitoring may require similar resources. Thus, clinicians should consider whether SDF or sealants are more cost-effective.
Cost-Effectiveness
Although the absolute effectiveness of sealants appears to be greater than that of SDF, the material and expert time has been estimated to be 20 times more for sealants than SDF.28 Indeed it has long been noted that sealants are more effective per tooth but much more expensive than SDF.14 In 2004 in Argentina, the cost-effectiveness of stabilizing one lesion with SDF was US$1.08.19 The increment of time for SDF treatment of four molars has been measured in a clinical trial adding 3.8 minutes.21 Thus, the incremental cost of a dental assistant paid $20 per hour to place SDF for prevention is $1.27, while a hygienist paid $50 per hour to place four sealants in 30 minutes costs $25, which is indeed 20 times more. The marginal improvement in clinical outcome from the significantly larger expense for sealants is questionable.
Esthetics
Mature enamel and non-carious dentin will not stain. However, any superficial defect in enamel-hypomineralized, carious/demineralized, and immature enamel-may stain black if it is sufficiently porous to allow penetration of significant amounts of silver. This includes early decay in fissures that may be difficult to see until it is stained as well as superficial defects from fluorosis. Subsurface defects of any type covered by mature enamel will not stain. Stains do indicate treatment of a defect in the tooth and are a very effective caries indicator, but may elicit cosmetic concerns. In most cases the stain from caries arrest in cavitated lesions can be handled (when desired) after minimal preparative cleaning of the cavosurface margins by placing an opaque dental material such as a high-viscosity glass-ionomer cement or resin opaquer. Similarly, stains in pits and fissures can be covered by an opaque material. Smooth non-cavitated surfaces, particularly in primary teeth, are less likely to hold these restorative materials.
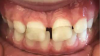
Application to erupting teeth in esthetic areas should be considered with caution. It is important to note that permanent teeth crowns can enter the mouth incompletely mineralized. While enamel always goes through a maturation process for years after eruption, in some patients (who do not have amelogenesis imperfecta) the emerging enamel is actually porous and takes at least a few weeks to close.29 This concern is compounded because enamel hypomineralization increases caries risk, and, thus, the children who would benefit most from the preventive effect are also at the highest risk for stain. Figure 3 shows an example of stain at the gingival margin when SDF was applied. The enamel surface gingival to the dark stain shows by contrast that all other exposed enamel may have been more subtly stained. The inciso-gingival thickness of the stain shows that the enamel was no longer susceptible to stain after being bathed in saliva for a few weeks.
Bonding
Various studies have documented that SDF does not affect the bond strength of glass-ionomer cement or resin to dentin.30-33 No published study has evaluated enamel bond strength.
Safety Considerations
Application of SDF to gingiva can cause desquamation without any sensation, akin to a bleach burn. If SDF touches a wound in the mucosa or a raw area of the tongue, it will sting. Blood fluoride levels do not rise above baseline in adults; thus, systemic exposure appears similar to a dose of toothpaste, not causing clinical risk of fluorosis.34
Dose Limit
Hypothetically, higher levels of systemic absorption may occur when using SDF for prevention rather than treatment. While SDF is almost completely absorbed into the tooth when applied to carious lesions, not as high of a proportion will be absorbed when applying to sound surfaces for prevention. This may increase the amount that will interact with the soft tissues and possibly be absorbed into the systemic circulation. Thus, increased doses should be justified, as in infants with early dental eruption and considerable caries risk.
Multiple-use vials and single-use (0.1 mL or two drops) ampules of SDF are available in the United States. The single-use ampules help prevent overdosing and spillage. The authors previously suggested a limit of one drop per 10 kg of body weight per visit, based on the esthetically pleasing 500-fold safety margin.22 This dose is in line with that evaluated in human safety studies34,35 and has been widely adopted in the United States.22,36 However, all indications show that it can be safely surpassed. Teeth tend to erupt very early in the populations who experience the highest prevalence of severe early childhood caries (eg, American Indian children). A dose limit that precludes beneficial use without being based on any real danger could indirectly cause suffering. The authors have found two drops to be adequate to wet the highest-risk surfaces of the primary dentition. Thus, until more clinical safety data are available, the authors suggest considering a dose limit of two drops per 10 kg per visit when using SDF for prevention. Thus, the dose limit is relevant primarily to infants and toddlers.
Recommended Application Protocol
Prior to application of SDF for prevention of new caries lesions, caregivers or patients should be properly informed of the risks, benefits, and alternatives of SDF as described previously.22 The noted risks should include photographs of SDF-induced stains, appropriate to prevention situations. The stated benefits should include a description of the size and number of new caries lesions anticipated without SDF and the difference in time, cost, and experience of the alternative treatments.
Prior to SDF application for prevention, prophylaxis is neither required nor advisable. Careful application of petroleum jelly (ie, Vaseline®) to protect the gingiva may be considered but petroleum jelly on the tooth surface will decrease effectiveness. Selected surfaces for prevention should be isolated with cotton, dried with cotton or compressed air, and one to two drops of SDF should be spread across all of the highest-risk surfaces in the mouth with a microbrush. Wetting of the surface is sufficient, and further isolation time for soaking in is not required. Excess should be removed with cotton. Some clinicians choose to cover treated areas with a varnish, such as a fluoride varnish, to prevent dilution by saliva.
Application Frequency
The only study found in this review that evaluated different application frequencies found no difference in outcomes between once or twice per year application in a population with a high caries rate of children.17 It is as yet unclear from available studies whether re-application of SDF is necessary to maintain the preventative effect of the first application, or if so, how often re-application is indicated. Annual reapplication of SDF has been found to be superior or equivalent to multiple applications per year of other contemporary topical preventives.6,16,24 Considering the patterns of clinical outcomes observed in the published trials in children, until more data is available the present authors suggest annual re-application. Because there is considerable evidence that risk factors correlate to incidence of new lesions, it would be logical to apply more frequently for patients with salivary dysfunction. Also, infants and toddlers with very high caries risk should be treated more frequently due to the rapid influx of high-risk surfaces.
Selection of Surfaces
SDF should be placed on the highest-risk surfaces as a priority. Usually, pits, fissures, and proximal surfaces have the highest risk. However, all surfaces are at similar risk in the upper anterior teeth of infants, exposed root surfaces bear the highest risk in older adults, and teenagers can suddenly develop proximal lesions on all posterior teeth. Thus, the pattern of lesions for the patient's demographics should be considered. Additionally, the patient's caries risk and esthetic concerns should be balanced in deciding which surfaces to treat.
Billing
SDF is a topical fluoride. Thus, D1208 is an appropriate billing code when SDF is used for prevention of new lesions. D1208 is typically billed as whole-mouth treatment. When SDF is used to stop the progression of enamel lesions into dentin, D1354 may be the most appropriate code. As of January 2018, D1354 is billed per tooth.
Conclusion
Considerable evidence supports the annual use of SDF for preventing new caries lesions in primary teeth and permanent molars. Multiple clinical trials show higher levels of prevention with less frequent applications of SDF than other topical therapies such as fluoride varnish. Considering all the evidence, the authors recommend annual application of SDF targeted to high-risk surfaces in high caries-risk patients of any age.
SDF seems to have a modestly less preventive effect but substantially greater cost-effectiveness than either resin or glass-ionomer cement sealants for preventing new lesions in permanent molars. SDF is also easier for patients to tolerate and can be more quickly applied than other preventive materials. Unlike sealants, SDF can be placed on any tooth surface, and the fluoride released may protect proximal surfaces not directly treated.
About the Authors
Jeremy A. Horst, DDS, PhD
Postdoctoral Scholar, Department of Biochemistry and Biophysics, University of California San Francisco, San Francisco, California; Private Practice, San Francisco, California
Masahiro Heima, DDS, PhD
Assistant Professor, Pediatric Dentistry, School of Dental Medicine, Case Western Reserve University, Cleveland, Ohio
Queries to the author regarding this course may be submitted to authorqueries@aegiscomm.com.
References
1. Chibinski AC, Wambier LM, Feltrin J, at al. Silver diamine fluoride has efficacy in controlling caries progression in primary teeth: a systematic review and meta-analysis. Caries Res. 2017;51(5):527-541.
2. Yamaga R, Nishino M, Yoshida S, Yokomizo I. Diammine silver fluoride and its clinical application. J Osaka Univ Dent Sch. 1972;12:1-20.
3. Nishino M. Studies on the topical application of ammoniacal silver fluoride for the arrest of dental caries. Osaka Daigaku Shigaku Zasshi. 1969;14(1):1-14.
4. Nishino M, Massler M. Immunization of caries-susceptible pits and fissures with a diammine silver fluoride solution. J Pedod. 1977;2(1):16-25.
5. Sato R, Saito Y. Clinical application of silver ammonia fluoride (Saforide) to children. Nippon Dental Review. 1970;332:66-67.
6. Chu CH, Lo EC, Lin HC. Effectiveness of silver diamine fluoride and sodium fluoride varnish in arresting dentin caries in Chinese pre-school children. J Dent Res. 2002;81(11):767-770.
7. Llodra JC, Rodriguez A, Ferrer B, et al. Efficacy of silver diamine fluoride for caries reduction in primary teeth and first permanent molars of schoolchildren: 36-month clinical trial. J Dent Res. 2005;84(8):721-724.
8. Gao SS, Zhao IS, Hiraishi N, et al. Clinical trials of silver diamine fluoride in arresting caries among children: a systematic review. JDR Clin Trans Res. 2016;1(3):201-210.
9. Rosenblatt A, Stamford TC, Niederman R. Silver diamine fluoride: a caries "silver-fluoride bullet. J Dent Res. 2009;88(2):116-125.
10. Almeida I, Bijella M, Lima J, et al. Evaluation of cariostatic and anticariogenic effects of 12% silver diaminofluoride (Bioride): longitudinal study. Rev Fac Odontol Bauru. 1994;2(4):28-30.
11. Medeiros UV, Miasato JM, de Almeida Monte Alto L, et al. Cariostatic and preventive effect of 30% silver fluoride diamine in infant patients. Braz J Dent. 1998;55(6):340-344.
12. Yoshida S, Okada M, Mori S, Baba H. Evaluation of topical application of diamine silver fluoride to pit and fissure of primary molars. J Gifu Dent Soc. 1976;4:35-41.
13. Tsutsumi N. Studies on topical application of Ag (NH3)2F for the control of interproximal caries in human primary molars: 3. Clinical trial of Ag(NH3)2F on interproximal caries in human primary molars. Jpn J Pediatr Dent. 1981;19(3):537-545.
14. Green E. A clinical evaluation of two methods of caries prevention in newly-erupted first permanent molars. Aust Dent J. 1989;34(5):407-409.
15. Monse B, Heinrich-Weltzien R, Mulder J, et al. Caries preventive efficacy of silver diammine fluoride (SDF) and ART sealants in a school-based daily fluoride toothbrushing program in the Philippines. BMC Oral Health. 2012;12:52. doi:10.1186/1472-6831-12-52.
16. Liu BY, Lo EC, Li CM. Effect of silver and fluoride ions on enamel demineralization: a quantitative study using micro-computed tomography. Aust Dent J. 2012;57(1):65-70.
17. Nguyen YHT, Ueno M, Zaitsu T, et al. Caries arresting effect of silver diamine fluoride in Vietnamese preschool children. Int J Clin Prev Dent. 2017;13(3):147-154.
18. Mattos-Silveira J, Floriano I, Ferreira FR, et al. New proposal of silver diamine fluoride use in arresting approximal caries: study protocol for a randomized controlled trial. Trials. 2014;15:448. doi:10.1186/1745-6215-15-448.
19. Mauro S, García Robles E, Cinque C, et al. Efficiency of three concentrated fluorides for the stabilization of enamel caries. Bol Asoc Argent Odontol Niños. 2004;33(2):4-11.
20. Braga MM, Mendes FM, De Benedetto MS, Imparato JC. Effect of silver diammine fluoride on incipient caries lesions in erupting permanent first molars: a pilot study. J Dent Child (Chic). 2009;76(1):28-33.
21. Mattos-Silveira J, Floriano I, Ferreira FR, et al. Children's discomfort may vary among different treatments for initial approximal caries lesions: preliminary findings of a randomized controlled clinical trial. Int J Paediatr Dent. 2015;25(4):300-304.
22. Horst JA, Ellenikiotis H, Milgrom PL. UCSF protocol for caries arrest using silver diamine fluoride: rationale, indications and consent. J Calif Dent Assoc. 2016;44(1):16-28.
23. Horst JA. Silver fluoride as a treatment for dental caries. Adv Dent Res. 2018;29(1):135-140.
24. Tan HP, Lo EC, Dyson JE, et al. A randomized trial on root caries prevention in elders. J Dent Res. 2010;89(10):1086-1090.
25. Marinho VC, Worthington HV, Walsh T, Clarkson JE. Fluoride varnishes for preventing dental caries in children and adolescents. Cochrane Database Syst Rev. 2013;(7):CD002279.
26. Yee R, Holmgren C, Mulder J, et al. Efficacy of silver diamine fluoride for arresting caries treatment. J Dent Res. 2009;88(7):644-647.
27. Policy on third-party reimbursement of fees related to dental sealants. Pediatr Dent. 2016;38(6):108-109.
28. dos Santos dos VE Jr, de Vasconcelos FM, Ribeiro AG, Rosenblatt A. Paradigm shift in the effective treatment of caries in schoolchildren at risk. Int Dent J. 2012;62(1):47-51.
29. Lynch RJ. The primary and mixed dentition, post-eruptive enamel maturation and dental caries: a review. Int Dent J. 2013;63 suppl 2:3-13.
30. Quock RL, Barros JA, Yang SW, Patel SA. Effect of silver diamine fluoride on microtensile bond strength to dentin. Oper Dent. 2012;37(6):610-616.
31. Selvaraj K, Sampath V, Sujatha V, Mahalaxmi S. Evaluation of microshear bond strength and nanoleakage of etch-and-rinse and self-etch adhesives to dentin pretreated with silver diamine fluoride/potassium iodide: an in vitro study. Indian J Dent Res. 2016;27(4):421-425.
32. Knight GM, McIntyre JM, Mulyani. The effect of silver fluoride and potassium iodide on the bond strength of auto cure glass ionomer cement to dentine. Aust Dent J. 2006;51(1):42-45.
33. Yamaga M, Koide T, Hieda T. Adhesiveness of glass ionomer cement containing tannin-fluoride preparation (HY agent) to dentin-an evaluation of adding various ratios of HY agent and combination with application diammine silver fluoride. Dent Mater J. 1993;12(1):36-44.
34. Vasquez E, Zegarra G, Chirinos E, et al. Short term serum pharmacokinetics of diammine silver fluoride after oral application. BMC Oral Health. 2012;12:60. doi:10.1186/1472-6831-12-60.
35. Milgrom P, Horst JA, Ludwig S, et al. Topical silver diamine fluoride for dental caries arrest in preschool children: a randomized controlled trial and microbiological analysis of caries associated microbes and resistance gene expression. J Dent. 2018;68:72-78. doi:10.1016/j.jdent.2017.08.015.
36. Crystal YO, Marghalani AA, Ureles SD, et al. Use of silver diamine fluoride for dental caries management in children and adolescents, including those with special health care needs. Pediatr Dent. 2017;39(5):135-145.