You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
In restorative practices, the largest category of restorations placed is typically the single-tooth direct placement restoration. The majority of these restorations are composite resins placed using adhesive bonding. According to the American Dental Association Survey Center’s 2005-2006 Survey of Dental Services Rendered, an estimated 146 million composite restorations and sealants were placed in the United States during the year-long survey.1 Heintze and Rousson estimated that more than 261 million direct composite resin restorations were placed worldwide in 2012.2
There has been a trend to teach the use of composite resin to restore posterior teeth.3 A recent survey of dental schools of single tooth direct posterior restorative materials revealed that of the 46 dental schools that responded to the survey, 63% no longer teach the use of amalgam as the favored restorative material when restoring posterior teeth.4 Christensen also reported that composite resins have surpassed amalgam as the material of choice for posterior restorations.5 With the trend to use composite resins in both the anterior and posterior regions for direct placement of single-tooth restorations, dentists find themselves using three primary types of materials: adhesives, composite resins, and light-curing devices. All three are critical to the success of the restoration. Even though this article will focus on the current state-of-the-art of resin adhesives, it is important that clinicians understand no one material or technique assures clinical success when placing restorations.
In recent years there have been advancements in the resin adhesives being used for direct placement composite resins. There are three major classes of resin adhesives: etch-and-rinse (total-etch), self-etch, and universal adhesives.6-8 The techniques for each of these adhesives are different and require attention to detail by the practitioner to achieve the desired clinical results. The trend for direct placement composite resin is the use of nano-hybrid and nano-filled composites.9,10 These composites have improved physical properties.
For both the resin adhesives and composite resins that are being used today in dental practices, the primary source of polymerization is light curing. Recently there has been concern that clinicians are not attending to the important aspects of light curing.11-13 Resin adhesives and composites have minimal light energy requirements to assure adequate photopolymerization. Although the techniques for light curing are better understood, the training of dentists and dental students needs to be improved to assure an adequate amount of light energy is delivered to restorations.12 With new technologies, light-curing devices can now be evaluated for a variety of parameters to ensure adequate energy delivery to restorations.14
Contemporary Adhesives
The adhesive placement of direct restorations is the standard in restorative dentistry. Nearly 60 years ago, Buonocore described the use of a diluted phosphoric acid liquid treatment to enamel to etch the surface, roughening it and creating microporosities that allowed an unfilled, self-cured acrylic resin to be retained.15 When the resin had polymerized, it mechanically locked to the enamel surface, forming small “tags” that extended into enamel microporosities that were 10- to 40-μm deep. The clinical success of enamel adhesive (bonding) has been well documented.16-18
Hard tissue tooth substrates that are prepared for restorations consist of both enamel and dentin. While enamel adhesion has been well established, the development of a dentin adhesive has been more challenging. Barkmeier described the fundamentals for predictable and successful bonding as such: the procedure must be safe and biologically acceptable; the level of bond strength must be clinically significant to avoid discoloration at the margins and prevent secondary caries; the bond strength must be reproducible so it can be routinely achieved at a predictable level for clinical success; the bond must be established quickly to allow for immediate finishing; and the bond must be clinically stable for a significant period of time.19
Whereas enamel is primarily a crystalline substrate with a composition by volume of 86% inorganic, 2% organic, and 10% water, dentin has more than twice the volume of water (25%) and a 25% organic component. The high volume of water within dentin’s tubular network created significant challenges for adhesion.20 The early generation bis-GMA resins used for enamel adhesion were hydrophobic and would not adequately wet the dentin.21 Also, there were early concerns that the use of phosphoric acid to etch dentin would cause pulpal inflammation and necrosis.22 Pulpal effects of phosphoric acid treated dentin were demonstrated to be minimal.23
A major breakthrough for the current generation of adhesives was the addition of a hydrophilic monomer, usually hydroxyethyl methacrylate (HEMA), to the hydrophobic monomer (bis-GMA). Rather than covering the dentin with a liner or base before etching, a simultaneous etch and rinse of the enamel and dentin with phosphoric acid followed by an adhesive application could now be predictably achieved.24-26 This work paralleled the investigations of dentin adhesion by Bowen.27
Current Classification of Adhesive Systems
The research and development of resin adhesives with a variety of chemistries and described techniques created some confusion to the clinician and researcher. Each product had unique instructions and, in some cases, names of the product category that could not be compared to other products that were being recommended.
It was not uncommon for manufacturers to describe the latest bonding agent based upon a generational timeline for development. The earliest adhesives, primarily enamel-only bonding agents, were referred to as first or second generation. The contemporary adhesives that required etching with phosphoric acid that combined HEMA with bis-GMA were being recommended for both enamel and dentin adhesion and were referred to as fourth- or fifth-generation systems. Yet research articles did not have a consistent labeling system. Fourth-generation bonding systems referred to use of phosphoric acid etching followed by a separate dentin primer and then adhesive resin painted on the etched dentin and enamel (multi-bottle). Fifth-generation bonding systems used the same phosphoric acid etchant but the primer and adhesive were combined in one bottle (single bottle). The earliest descriptions of these adhesives used the term total etch.
As for any dental restorative technique and material, the tooth needs to be well isolated to avoid contamination during restoration placement. Without adequate isolation the duration of a procedure, a number of steps can compromise the durability of the restoration placed. With this in mind, clinicians desired a more simplified approach with fewer steps. The goal of minimizing the number of steps stimulated research in the development of self-etching bonding systems. These self-etching adhesives eliminated the pretreatment of the enamel and dentin with phosphoric acid by incorporating acidic monomer in the primer or into the primer/adhesive components.6 These new systems were referred to as sixth generation (multi-bottle self-etch adhesives) and seventh generation (single-bottle self-etch adhesives).
Whether an adhesive requires a separate etching step with phosphoric acid or uses an acidic primer, the surface treatment result of the enamel and dentin is similar.28 Van Meerbeek and colleagues described a rational classification of resin adhesives based upon the technique for surface treatment before composite placement (Table 1).7 At the time, there were two distinct categories, etch and rinse (separate use of phosphoric acid etching pretreatment of the tooth surface) and self-etch. In recent years several manufacturers have introduced a hybrid of an etch-and-rinse and self-etch system, now referred to as a universal adhesive.8,29 Clinical applications for all resin adhesives are product specific and based upon the instructions for use for each adhesive (Table 2).30
Etch and Rinse
Etch and rinse refers to any adhesive system that requires a pretreatment of the tooth structure with a phosphoric acid etchant prior to adhesive application. The etchant is rinsed from the tooth surfaces with a water or air-water spray. The tooth is then dried. The etch-and-rinse technique leaves an enamel surface that is morphologically microscopically roughened to allow for a mechanical bond between the enamel and dentin and the adhesive. The 10% to 40% phosphoric acid etchant removes the smear layer of the enamel and dentin that was created by the tooth preparation. Etch-and-rinse adhesives are supplied as either multi-bottle systems, with separate bottles for the dentin primer (solvent and HEMA) and the adhesive resin (referred to as a three-step etch and rinse), or as a single bottle that contains both dentin primer and adhesive resin (referred to as a two-step etch and rinse). Many of the adhesive systems are provided as bulk bottles or unit-dose applications. For three-step etch-and-rinse adhesives, the dentin is rewetted with water before adhesive application, leaving a slightly damp, glossy surface. For many two-step etch-and-rinse adhesives, there is water in the adhesive and no need to moisturize the dentin.31-33 In vitro and in vivo research have shown that etch-and-rinse adhesives can reliably bond to enamel and dentin.34-36
Self-Etch
Self-etch adhesive systems provide a simplification to the adhesive process by eliminating the separate etching step and the rinsing and drying of the tooth structure. Self-etch adhesives use an acidic monomer in a HEMA/water-based adhesive to etch the tooth surface. The acidic monomer can be incorporated into a separate self-etch primer and resin adhesive, a two-step self-etch adhesive, or a single-step application of the self-etch adhesive. Single-step application adhesives are found in two different forms: a single bottle or two components that require mixing prior to a single-step application. Many of the one-step self-etch products are available in unit dosing. Self-etch adhesives contain water so there is no need for a dentin rewetting step during restoration.31-33 Clinicians should be aware of the instructions for use from the manufacturer when selecting clinical applications of the self-etch adhesive systems. Resin adhesion to dentin involves the resin penetrating the dentin after etching. Research has shown the self-etch adhesives provide equivalent resin hybridization and infiltration of the dentin as what has been reported with etch-and-rinse adhesive systems. There has been concern about the ability of a self-etch adhesive system to adequately etch the enamel surface and provide retentive adhesion to enamel. Self-etch adhesives are less aggressive at etching enamel than the pretreatment of enamel with a phosphoric acid etchant when the enamel morphology was viewed with microscopy.37,38 The morphology of the etched enamel and the adhesive interface is product dependent and does not translate into a reduced enamel bond.38-41
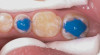
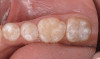
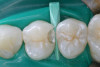
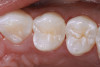
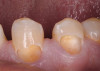
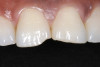
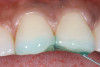
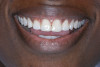
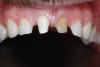
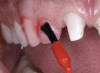
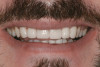
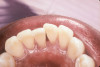
Based on the current clinical evidence, it has been recommended that a self-etch adhesive is clinically accepted for restoring Class I, II, III, and V restorations; currently, etch-and-rinse adhesives can be used for all classes of direct placement restorations, as well as sealant placement, restoring Class IV incisal edge fractures, esthetic facial veneering and diastema closures with direct composite resin, bonding porcelain veneers, and fiber-reinforced splints (clinical examples are shown in Figure 1 through Figure 14).18,42-48 As more clinical evidence becomes available, these recommendations can change. Self-etch adhesives can be used for primarily enamel adhesion and retention using a selective etching technique.45,49
Universal
Universal adhesives have been introduced by manufacturers in the past few years to address the ability of self-etch adhesives to adequately etch enamel surfaces. These universal adhesives are a combination of a self-etch adhesive and an etch-and-rinse adhesive for enamel bonding clinical applications. Universal adhesives recommend etching the enamel as a separate step and treating the dentin with the self-etch capacity of the universal adhesive system.8,29,50-52
Understanding for Improved Tooth Adhesion
In clinical practice, there is variation in the surface structure of enamel and dentin encountered. Teeth are restored due to the presence of pathology and changes to the tooth surfaces. Teeth are attacked by caries or there is the presence of defective restorations that require retreatment. The quality of the enamel and dentin can affect the adhesive interface.
Considerations for Dentin
There has been concern of a continuous degradation of dentin adhesion over time and a wide variation of dentin bonding effectiveness among systems.53-61 Auto-degradation of collagen matrices with the hybrid layers created by the slow action of matrix metalloproteinases (MMPs) has been reported with both etch-and-rinse and self-etch contemporary adhesives.60-62 To combat this degradation, a number of different strategies using cross-linking agents, eg, chlorhexidine (CHX), have been successfully used to inhibit MMPs.62-65 The use of a 2% CHX conditioner has been shown to be effective in inhibiting dentin-bonding degradation.66,67 Other MMP inhibitors, quaternary ammonium methacrylates, benzalkonium chloride, and carbodiimide, have also been effective in stabilizing dentin adhesion.68-70 The addition of MMPs inhibitors directly to a self-etch adhesive has also been demonstrated to be effective in stabilizing dentin adhesion.71
The structure of enamel and dentin can have an impact on treatment recommendations. In most instructions for use for etch and rinse adhesives, enamel is etched for 15 to 30 seconds and dentin for 15 seconds. Recent research has shown that normal dentin of younger patients has a different structure than dentin of older patients (aged 55 to 60 years and older).72,73 These studies recommend an increase in etching time of 30 seconds for sclerotic dentin.
Dental fluorosis is a hypomineralization of enamel resulting from excessive ingestion of fluoride during tooth development. The enamel appears mottled with small white streaks. Dental fluorosis has been reported at frequencies of 36.1% for 16- to 19-year-olds and 28.4% among 20- to 29-year-olds.74 Fluorosed enamel and dentin are more resistant to etching and adhesion than normal enamel and dentin. To enhance bonding for fluorosed enamel, it is recommended that the enamel be prepared with a bur or diamond.75 Self-etch adhesives provide better bonding to fluoride-rich dentin.76
Discolored dentin can be a result of residual caries, caries affected dentin, or amalgam discoloration. The complete removal of caries or caries-affected dentin has been controversial. Indirect pulp capping is an accepted dental practice.72 The use of caries-detecting dyes has been recommended by some to visualize caries so it can be removed. Yet the presence of caries-detecting dye impacts dentin adhesive negatively.78,79 In addition, adhesion values to caries-affected dentin are lower than to normal dentin.80,82 It is not uncommon to visualize darkly discolored dentin under an existing amalgam restoration after its removal. This discolored dentin is caused by the metallic ions and corrosion particles that have invaded the dentinal tubules. Harnirattisai and colleagues reported the adhesion to normal dentin and amalgam-affected dentin with both etch-and-rinse adhesive and self-etch adhesive was equivalent.83
Tooth Whitening
Tooth whitening is a very well accepted esthetic treatment modality. In-office professional whitening procedures provide the clinician with control over the bleaching process. With either at-home bleaching trays, whitening strips, and other over-the-counter techniques, the patient may be whitening their teeth with a hydrogen peroxide or carbamide peroxide bleaching agent. Studies investigating resin adhesion and bleaching have reported that waiting at least 1 week after bleaching with an active peroxide agent is necessary to prevent any negative consequences when using either an etch-and-rinse or self-etch bonding agent.84-86 Also, there is concern that postoperative peroxide bleaching will have a negative impact by degrading the adhesive interface with composite resin.87,88
Self-Cure/Dual-Cure Composites
Even though the majority of direct placement composite resins are light cured, there is still a predominant use of self-cure and dual-cured composite resins as core foundations for fixed prosthodontics. Recent inquiry has focused on the compatibility of etch-and-rinse single-bottle and self-etch adhesives with self-cure and dual-cure composite core composites. There is contradictory evidence on the ability of etch-and-rinse single-bottle adhesives and self-etch adhesives to create an adequate resin interface to resist the forces of occlusion.89-92 In the past 5 years, chemical additives have been introduced to address this concern. It is the responsibility of the clinician to review the instructions for use of an adhesive to identify its compatibility with self-cure and dual-cure composite resins.
Conclusion
Clinicians have seen the introduction of a wide variety of adhesive systems over the past 3 decades. The complexities in the instructions for use of many of the bonding systems used require an attention to detail. It is not as easy as paint on and light cure. Each product requires attention to the instructions for application, agitation, time leaving the product on the tooth, air drying, and light curing. Do not take it for granted that a new bonding system is meant to be used the same as one you have used in the past, even if it is from the same manufacturer.
Simplified systems have been introduced in recent years that provide the etching, primer, and adhesive all in one. A clinician needs to evaluate the clinical requirements of an adhesive restorative system he or she selects for restoring the natural dentition. To help with the decision to make a change in the adhesive being used, ask the manufacturer to provide additional information on not only in vitro research but also clinical trials. Whichever system the clinician selects, he or she should follow a manufacturer’s recommendations for clinical applications to ensure clinical success.
References
1. American Dental Association Survey Center. 2005-2006 Survey of Dental Services Rendered. Chicago: American Dental Association; 2007:1-181.
2. Heintze SD, Rousson V. Clinical effectiveness of direct class II restorations - a meta-analysis. J Adhes Dent. 2012;14(5):407-431.
3. Lynch CD, Frazier KB, McConnell RJ, et al. Minimally invasive management of dental caries: contemporary teaching of posterior resin-based composite placement in U.S. and Canadian dental schools. J Am Dent Assoc. 2011;142(6):612-620.
4. Liew Z, Nguyen E, Stella R, et al. Survey on the teaching and use in dental schools of resin-based materials for restoring posterior teeth. Int Dent J. 2011;61(1):12-18.
5. Christensen GJ. Should resin-based composite dominate restorative dentistry today? J Am Dent Assoc. 2010;141(12):1490-1493.
6. Ozer F, Blatz MB. Self-etch and etch-and-rinse adhesive systems in clinical dentistry. Compend Contin Educ Dent. 2013;34(1):12-30.
7. Van Meerbeek B, De Munck J, Yoshida Y, et al. Buonocore memorial lecture. Adhesion to enamel and dentin: current status and future challenges. Oper Dent. 2003;28(3):215-235.
8. Perdigão J, Loguercio AD. Universal or Multi-mode Adhesives: Why and How? J Adhes Dent. 2014;16(2):193-194.
9. Palaniappan S, Elsen L, Lijnen I, et al. Nanohybrid and microfilled hybrid versus conventional hybrid composite restorations: 5-year clinical wear performance. Clin Oral Investig. 2012;16(1):181-190.
10. Sensi LG, Strassler HE, Webley W. Direct composite resins. Inside Dentistry. 2007;3(7):76-79.
11. Ferracane J, Watts DC, Barghi N, et al. Effective use of dental curing lights: a guide for the dental practitioner. J Am Dent Assoc (PPR supplement). 2013;8(2):2-12.
12. Price RB, Strassler HE, Price HL, et al. The effectiveness of using a patient simulator to teach light-curing skills. J Am Dent Assoc. 2014;145(1):32-43.
13. Santini A, Turner S. General dental practitioners’ knowledge of polymerisation of resin-based composite restorations and light curing unit technology. Br Dent J. 2011;211(6):E13.
14. Price RB, Shortall AC, Palin WM. Contemporary issues in light curing. Oper Dent. 2014;39(1):4-14.
15. Buonocore MG. A simple method of increasing the adhesion of acrylic filling materials to enamel surfaces. J Dent Res. 1955;34(6):849-853.
16. Torney DL, Denehy GE, Teixeira LC. The acid-etch class III composite resin restoration. J Prosthet Dent. 1977;38(6):623-626.
17. Jordan RE, Suzuki M, Gwinnett AJ, Hunter JK. Restoration of fractured and hypoplastic incisors by the acid etch resin technique: a three-year report. J Am Dent Assoc. 1977;95(4):795-803.
18. Strassler HE. Applications of total-etch adhesive bonding. Compend Contin Educ Dent. 2003;24(6):427-441.
19. Brudevold F, Buonocore M, Wileman W. A report on a resin composition capable of bonding to human dentin surfaces. J Dent Res. 1956;35(6):846-851.
20. Van Meerbeek B, Inoue S, Perdigão J, et al. Enamel and dentin adhesion. In: Summitt JB, Robbins JW, Schwartz RS, eds. Fundamentals of Operative Dentistry a Contemporary Approach. 2nd ed. Hanover Park, IL: Quintessence Books; 2001:178-235.
21. Torney DL, Denehy GE, Teixeira LC. The acid-etch class III composite resin restoration. J Prosthet Dent. 1977;38(6):623-626.
22. Skinner EW, Phillips RW. The Science of Dental Materials. 5th ed. Philadelphia, PA: WB Saunders; 1960:277.
23. Jennings RE, Ranly DM. Autoradiographic studies of 32 P penetration into enamel and dentin during acid etching. ASDC J Dent Child. 1972;39(1):69-71.
24. Fusayama T, Nakamura M, Kurosaki N, Iwaku M. Non-pressure adhesion of a new adhesive restorative resin. J Dent Res. 1979;58(4):1364-1370.
25. Bertolotti RL. Acid etching of dentin. Quintessence Int. 1990; 21:77-78.
26. Kanca J 3rd. One-year evaluation of a dentin-enamel bonding system. J Esthet Dent. 1990;2(4):100-103.
27. Bowen RL, Cobb EN. A method for bonding to dentin and enamel. J Am Dent Assoc. 1983;107(5):734-736.
28. Van Meerbeek B. Mechanism of resin adhesion: dentin and enamel bonding. Functional Esthet Restor Dent. 2008; 2(1):18-25.
29. Wagner A, Wendler M, Petschelt A, et al. Bonding performance of universal adhesives in different etching modes. J Dent. 2014;42(7):800-807.
30. Strassler HE, Mann M. Dental adhesives for direct placement composite. IndeedCE.com website. www.ineedce.com/courses/2192/PDF/1108cei_dentsply_Adhesives.pdf. Accessed August 19, 2014.
31. Hegde MN, Manjunath J. Bond strength of newer dentin bonding agents in different clinical situations. Oper Dent. 2011;36(2):169-176.
32. Pucci CR, de Oliveira RS, Caneppele TM, et al. Effects of surface treatment, hydration and application method on the bond strength of a silorane adhesive and resin system to dentine. J Dent. 2013;41(3):278-286.
33. Caneppele TM, Torres CR, Sassaki A, et al. Effects of surface hydration state and application method on the bond strength of self-etching adhesives to cut enamel. J Adhes Dent. 2012;14(1):25-30.
34. Peumans M, Kanumilli P, De Munck J, et al. Clinical effectiveness of contemporary adhesives: a systematic review of current clinical trials. Dent Mater. 2005;21(9):864-881.
35. Inoue S, Vargas MA, Abe Y, et al. Microtensile bond strength of eleven contemporary adhesives to enamel. Am J Dent. 2003;16(5):329-334.
36. Shirai K, De Munck J, Yoshida Y, et al. Effect of cavity configuration and aging on the bonding effectiveness of six adhesives to dentin. Dent Mater. 2005;21(2):110-124.
37. Perdigão J, Geraldeli S. Bonding characteristics of self-etching adhesives to intact versus prepared enamel. J Esthet Restor Dent. 2003;15(1):32-41; discussion 42.
38. Abdalla AI, El Zohairy AA, Abdel Mohsen MM, Feilzer AJ. Bond efficacy and interface morphology of self-etching adhesives to ground enamel. J Adhes Dent. 2010;12(1):19-25.
39. Senawongse P, Sattabanasuk V, Shimada Y, et al. Bond strengths of current adhesive systems on intact and ground enamel. J Esthet Restor Dent. 2004;16(2):107-115; discussion 116.
40. Yazici AR, Yildirim Z, Ertan A, et al. Bond strength of one-step self-etch adhesives and their predecessors to ground versus unground enamel. Eur J Dent. 2012;6(3):280-286.
41. Brackett WW, Ito S, Nishitani Y, et al. The microtensile bond strength of self-etching adhesives to ground enamel. Oper Dent. 2006;31(3):332-337.
42. Strassler HE. Self-etching resin adhesives. Inside Dentistry. 2007;3(2):50-53.
43. Karaman E, Yazici AR, Tuncer D, et al. A 48-month clinical evaluation of fissure sealants placed with different adhesive systems. Oper Dent. 2013;38(4):369-375.
44. Peumans M, Kanumilli P, De Munck J, et al. Clinical effectiveness of contemporary adhesives: a systematic review of current clinical trials. Dent Mater. 2005;21(9):864-881.
45. Peumans M, De Munck J, Van Landuyt K, et al. Five-year clinical effectiveness of a two-step self-etching adhesive. J Adhes Dent. 2007;9(1):7-10.
46. Krithikadatta J. Clinical effectiveness of contemporary dentin bonding agents. J Conserv Dent. 2010;13(4):173-183.
47. van Dijken JW, Pallesen U. A 7-year randomized prospective study of a one-step self-etching adhesive in non-carious cervical lesions. The effect of curing modes and restorative material. J Dent. 2012;40(12):1060-1067.
48. van Dijken JW. A randomized controlled 5-year prospective study of two HEMA-free adhesives, a 1-step self etching and a 3-step etch-and-rinse, in non-carious cervical lesions. Dent Mater. 2013;29(11):e271-e280.
49. Frankenberger R, Lohbauer U, Roggendorf MJ, et al. Selective enamel etching reconsidered: better than etch-and-rinse and self-etch? J Adhes Dent. 2008;10(5):339-344.
50. Wagner A, Wendler M, Petschelt A, et al. Bonding performance of universal adhesives in different etching modes. J Dent. 2014;42(7):800-807.
51. Muñoz MA, Luque I, Hass V, et al. Immediate bonding properties of universal adhesives to dentine. J Dent. 2013;41(5):404-411.
52. Perdigão J, Kose C, Mena-Serrano AP, et al. A new universal simplified adhesive: 18-month clinical evaluation. Oper Dent. 2014;39(2):113-127.
53. De Munck J, Van Landuyt K, Peumans M, et al. A critical review of the durability of adhesion to tooth tissue: methods and results. J Dent Res. 2005;84(2):118-132.
54. De Munck J, Van Meerbeek B, Yoshida Y, et al. Four-year water degradation of total-etch adhesives bonded to dentin. J Dent Res. 2003;82(2):136-140.
55. Meiers JC, Young D. Two-year composite/dentin bond stability. Am J Dent. 2001;14(3):141-144.
56. García-Godoy F, Tay FR, Pashley DH, et al. Degradation of resin-bonded human dentin after 3 years of storage. Am J Dent. 2007;20(2):109-113.
57. Pashley DH, Tay FR, Yiu C, et al. Collagen degradation by host-derived enzymes during aging. J Dent Res. 2004;83(3):216-221.
58. Koshiro K, Inoue S, Tanaka T, et al. In vivo degradation of resin-dentin bonds produced by a self-etch vs. a total-etch adhesive system. Eur J Oral Sci. 2004;112(4):368-375.
59. Osorio R, Pisani-Proenca J, Erhardt MC, et al. Resistance of ten contemporary adhesives to resin-dentine bond degradation. J Dent. 2008;36(2):163-169.
60. Moon PC, Weaver J, Brooks CN. Review of matrix metalloproteinases’ effect on the hybrid dentin bond layer stability and chlorhexidine clinical use to prevent bond failure. Open Dent J. 2010;4:147-152.
61. Mazzoni A, Scaffa P, Carrilho M, et al. Effects of etch-and-rinse and self-etch adhesives on dentin MMP-2 and MMP-9. J Dent Res. 2013;92(1):82-86.
62. Montagner AF, Sarkis-Onofre R, Pereira-Cenci T, Cenci MS. MMP Inhibitors on dentin stability: A systematic review and meta-analysis. J Dent Res. 2014;93(8):733-743.
63. Scheffel DL, Hebling J, Scheffel RH, et al. Inactivation of matrix-bound matrix metalloproteinases by cross-linking agents in acid-etched dentin. Oper Dent. 2014;39(2):152-158.
64. Breschi L, Cammelli F, Visintini E, et al. Influence of chlorhexidine concentration on the durability of etch-and-rinse dentin bonds: a 12-month in vitro study. J Adhes Dent. 2009;11(3):191-198.
65. Toledano M, Yamauti M, Osorio E, et al. Influence of dentin etching on MMP mediated collagen degradation [abstract]. J Dent Res (IADR abstracts). 2011;90. Abstract 1146.
66. Stanislawczuk R, Amaral RC, Zander-Grande C, et al. Chlorhexidine-containing acid conditioner preserves the longevity of resin-dentin bonds. Oper Dent. 2009;34(4):481-490.
67. Stanislawczuk R, Reis A, Loguercio AD. A 2-year in vitro evaluation of a chlorhexidine-containing acid on the durability of resin-dentin interfaces. J Dent. 2011;39(1):40-47.
68. Sabatini C, Patel SK. Matrix metalloproteinase inhibitory properties of benzalkonium chloride stabilizes adhesive interfaces. Eur J Oral Sci. 2013;121(6):610-616.
69. Mazzoni A, Apolonio FM, Saboia VP, et al. Carbodiimide inactivation of MMPs and effect on dentin bonding. J Dent Res. 2014;93(3):263-268.
70. Tezvergil-Mutluay A, Agee KA, Uchiyama T, et al. The inhibitory effects of quaternary ammonium methacrylates on soluble and matrix-bound MMPs. J Dent Res. 2011;90(4):535-540.
71. Zhou J, Tan J, Yang X, et al. Effect of chlorhexidine application in a self-etching adhesive on the immediate resin-dentin bond strength. J Adhes Dent. 2010;12
(1):27-31.
72. Lopes GC, Baratieri CM, Baratieri LN, et al. Bonding to cervical sclerotic dentin: effect of acid etching time. J Adhes Dent. 2004;6(1):19-23.
73. Lopes GC, Vieira LC, Araújo E, et al. Effect of dentin age and acid etching time on dentin bonding. J Adhes Dent. 2011;13(2):139-145.
74. Beltrán-Aguilar ED, Barker L, Dye BA. Prevalence and severity of dental fluorosis in the United States, 1999-2004. NCHS Data Brief. 2010;(53):1-8.
75. Ermis RB, De Munck J, Cardoso MV, et al. Bonding to ground versus unground enamel in fluorosed teeth. Dent Mater. 2007;23(10):1250-1255.
76. Waidyasekera PG, Nikaido T, Weerasinghe DD, Tagami J. Bonding of acid-etch and self-etch adhesives to human fluorosed dentine. J Dent. 2007;35(12):915-922.
77. Strassler HE, Levin R. Vital pulp therapy with pulp capping. Dent Today. 2012;31(11):98-105.
78. Singh UP, Tikku A, Chandra A, et al. Influence of caries detection dye on bond strength of sound and carious affected dentin: An in-vitro study. J Conserv Dent. 2011;14(1):32-35.
79. Demarco FF, Matos AB, Matson E, Powers JM. Dyes for caries detection influence sound dentin bond strength. Oper Dent. 1998;23(6):294-298.
80. Ceballos L, Camejo DG, Victoria Fuentes M, et al. Microtensile bond strength of total-etch and self-etching adhesives to caries-affected dentine. J Dent. 2003;31(7):469-477.
81. Omar H, El-Badrawy W, El-Mowafy O, et al. Microtensile bond strength of resin composite bonded to caries-affected dentin with three adhesives. Oper Dent. 2007;32(1):24-30.
82. Scholtanus JD, Purwanta K, Dogan N, et al. Microtensile bond strength of three simplified adhesive systems to caries-affected dentin. J Adhes Dent. 2010;12(4):273-278.
83. Microtensile bond strengths of two adhesive resins to discolored dentin after amalgam removal. J Dent Res. 2007;86(3):232-236.
84. Godwin JM, Barghi N, Berry TG, et al. Time duration for dissipation of bleaching effects before enamel bonding [abstract]. J Dent Res. 1992;71:179. Abstract 590.
85. Basting RT, Rodrigues JA, Serra MC, Pimenta LA. Shear bond strength of enamel treated with seven carbamide peroxide bleaching agents. J Esthet Restor Dent. 2004;16(4):250-260.
86. Braz R, Cordeiro-Loretto S, de Castro-Lyra AM, et al. Effect of bleaching on shear bond strength to dentin of etch-and-rinse and self-etching primer adhesives. Acta Odontol Latinoam. 2012;25(1):20-26.
87. Dudek M, Roubickova A, Comba L, et al. Effect of postoperative peroxide bleaching on the stability of composite to enamel and dentin bonds. Oper Dent. 2013;38(4):394-407.
88. Roubickova A, Dudek M, Comba L, et al. Effect of postoperative peroxide bleaching on the marginal seal of composite restorations bonded with self-etch adhesives. Oper Dent. 2013;38(6):644-654.
89. Pascuita M, Cobb D, Denehy G. Shear bond strength of dual cure primer/adhesives with dual cure resin cements [abstract]. J Dent Res (Special Issue A). 2002; 81:A-76. Abstract 405.
90. Cheong C, King NM, Pashley DH, et al. Incompatibility of self-etch adhesives with chemical/dual-cured composites: two-step vs one-step systems. Oper Dent. 2003;28(6):747-755.
91. Tay FR, Pashley DH, Yiu CK, et al. Factors contributing to the incompatibility between simplified-step adhesives and chemically-cured or dual-cured composites. Part I. Single-step self-etching adhesive. J Adhes Dent. 2003;5(1):27-40.
92. King N, Tay F, Pashley DH, et al. Incompatiblity profiles of all-in-one adhesives: 1. True vs apparent incompatibility [abstract]. J Dent Res (IADR abstracts). 2004;83. Abstract 23.
About the Author
Howard E. Strassler, DMD
Professor and Director of Operative Dentistry
Department of Endodontics, Prosthodontics, and Operative Dentistry
Baltimore, Maryland